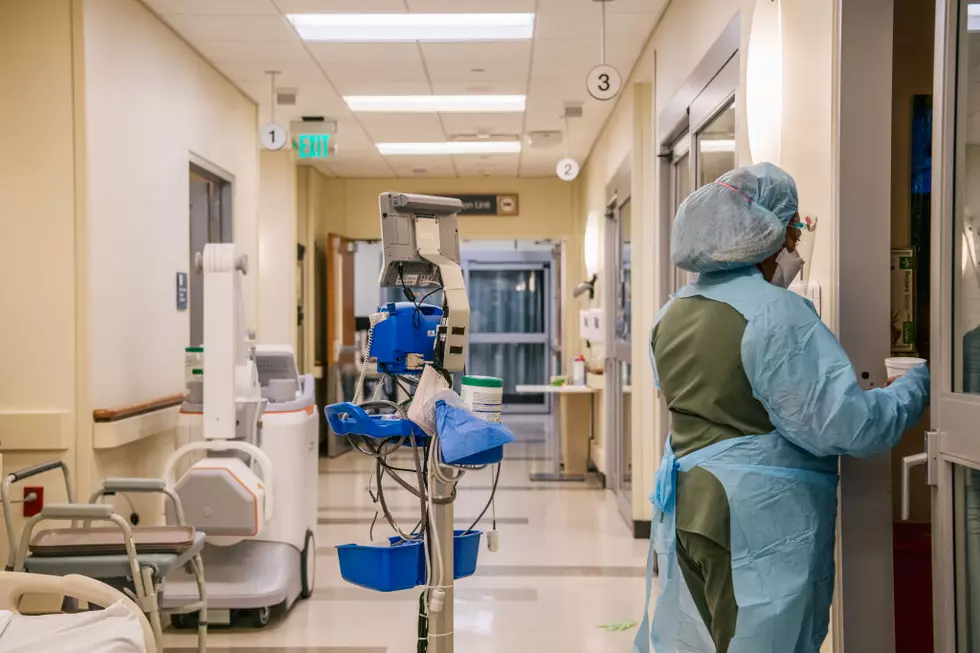
WSDOH School Re-Open Guidance Mentions “Structural Racism”
It's a dizzying list of requirements, "guidance" and information for school districts in WA State, from the Washington State Department of Health.
The document, dated August 4, 2020, is entitled "K-12 Schools, Fall 2020-2021 Guidance."
It's the guide for how schools 'have' to proceed if they are to open for in class education. It reads in similar fashion to what businesses are expected to do with COVID, but far more in depth.
We strongly encourage you read it for yourself. What jumped out at us was on Page 12. Under the section of "More COVID-19 information and resources," the following paragraph is included. This is it verbatim:
"A person’s race/ethnicity or nationality does not, itself, put them at greater risk of COVID-19. However, data are revealing that communities of color are being disproportionately impacted by COVID-19- this is due to the effects of racism, and in particular, structural racism, that leaves some groups with fewer opportunities to protect themselves and their communities. Stigma will not help to fight the illness. Share accurate information with others to keep rumors and misinformation from spreading." (Bold lettering added for emphasis).
This is in the guide sent to all school districts in WA, for how to approach openings concerning COVID-19.
It is rather lengthy, but we have included it below. It is presented in this format because of limitations with inserting a link to document site.
K-12 Schools – Fall 2020-2021 Guidance
Schools are fundamental to child and adolescent development and well-being and provide our children and adolescents with academic instruction, social and emotional skills, safety, reliable nutrition, physical/speech and mental health therapy, and opportunities for physical activity, among other benefits.
This guidance strives to provide feasible actions schools can take to mitigate risks to student and staff from COVID-19 and allow schools to resume in-person instruction whether full time for all students, phased, or hybrid models of partial online and partial in-person instruction.
This guidance is specific to K-12 public or private schools regardless of what phase or county they are in. Use this guidance to inform how to resume in person school and the accompanying document, “K-12 School Decision Tree” for decisions about when/if to resume in person school.
All decisions should be made in coordination with the local school board and the local health department.
The following guidance incorporates information from CDC Interim Guidance for Administrators of US K-12 Schools and Child Care Programs--Plan, Prepare, and Respond to Coronavirus Disease 2019 (COVID-19), K-12 Schools and Child Care Programs and CDC COVID-19 Considerations for Schools. It is intended to assist schools in complying with Governor and Office of Superintendent of Public Instruction (OSPI) requirements to help ensure employee and student safety during the COVID-19 pandemic.
Promoting health and safety in schools relies on communication between schools and local public health authorities. FERPA allows schools to share personally identifiable information with local public health authorities without consent, including parental consent, when needed to respond to a health emergency
(https://studentprivacy.ed.gov/sites/default/files/resource_document/file/FERPA%20and%20 Coronavirus%20Frequently%20Asked%20Questions_0.pdf). If the school buildings have been shuttered, please follow CDC guidance on safely reopening the buildings:
Reopening Buildings after Shutdown. This guidance is based on existing science, expert public health opinion, current policies, and stakeholder input. This guidance does not address extracurricular activities, such as youth sports. When in person learning resumes, refer to Washington Interscholastic Activities Association (WIAA) for specific guidance for sport (https://www.wiaa.com/default.aspx?SecID=46).
2 Key Principles for Reducing Potential Exposures The mainstays of reducing exposure to the coronavirus and other respiratory pathogens are: • Keep ill persons out of school — educating students, families and staff to stay home when sick, and using screening • Cohorts — conducting all activities in small groups that remain together over time with minimal mixing of groups. • Physical distancing — minimizing close contact (less than six feet) with other people. • Hand hygiene — frequent washing with soap and water or using alcohol-based hand gel. • Protective equipment — use of face coverings or shields, and barriers. • Environmental cleaning and disinfection — especially of high-touch surfaces. • Improve indoor ventilation • Isolation of sick people and exclude exposed people. • With the above considerations foremost, outdoor activities are safer than indoor activities. Based on these principles, everyone should understand that more, closer, and longer interactions between people is associated with more risk of COVID-19.
Risk of COVID-19 spread increases in school settings as follows: • Lowest Risk: Students and teachers engage in virtual-only classes, activities, and events. • More Risk: Small, in-person classes, activities, and events. Groups of students stay together and with the same teacher throughout/across school days, and groups do not mix. Students remain at least six feet apart and do not share objects (e.g., hybrid virtual and in-person class structures, or staggered/rotated scheduling to accommodate smaller class sizes). • Highest Risk: Full sized, in-person classes, activities, and events. Students are not spaced apart, share classroom materials or supplies, and mix between classes and activities.
General Guidance Do not allow students, staff, vendors, parents and guardians, or guests on-site if they: 1. Are showing symptoms of COVID-19. 2. Have been in close contact* (within 6 feet for at least 15 minutes) with someone who has confirmed COVID-19 in the last 14 days. 3. Have tested positive for COVID-19 in the past 10 days DOH recognizes the need to plan ahead while the science of COVID-19 evolves. Further, the trajectory of disease in our state and nation may require changes to our state’s response including in schools. DOH will update this guidance and the K-12 decision tree periodically and work with OSPI to ensure districts, schools, and families are aware of updates.
3 *Health care providers, EMS workers, and staff who wore proper personal protective equipment (PPE) during potential COVID-19 exposure are permitted to be in site. Ensure staff are trained in health and safety protocols for your site, including how to screen for symptoms, maintaining physical distance, wearing appropriate PPE, importance of frequent cleaning and handwashing, and what to do if someone develops signs of COVID-19. Communicate regularly with students, families and staff, and emphasize the importance of staying home when sick, physical distancing of six feet, and hand hygiene. Communication should be provided using multiple modalities (posters, written hard copy, email, text message, phone, video conferencing) and in languages that parents best understand. All students age 5 years and older, staff, volunteers, and guests must wear cloth face coverings (or other acceptable alternative) in K-12 settings.
See below for more information about cloth face coverings guidance. In addition, schools have a general obligation to provide employees a safe and healthy work site in accordance with state and federal law and safety and health rules, including addressing hazards associated with COVID-19. Refer to the Department of Labor & Industries’ COVID-19 Workplace Safety and Health Requirements for more information.
Monitor student and employee attendance and absences, have flexible locally-determined leave policies and practices, and have access to trained substitutes to support employee absences. People at High Risk for Serious Health Problems from COVID-19 Those at high risk for health problems from COVID-19 should consult with their health care provider when considering whether to provide or participate in K-12 activities.
Protections for employees at high risk for health problems remain in place under Proclamation 20-46. Families with a member who is at high risk from COVID-19 should carefully consider risks and benefits of sending their student to in person school. Drop-Off and Pick-Up Develop a system for drop-off and pick-up that keeps families at least six feet from each other and reduces their need to enter the school. This may include staggering drop-off and pick-up times for various groups, one-way traffic flows, greeting students at their vehicle, or placing distancing markers on walkways. Health Screening at Entry Staff and students with any illness must stay home. Students and staff should be assessed for illness before attending school each day. Encourage parents to be on the alert for signs of illness in their children and to keep them home when they are sick. Screen children upon arrival, if possible.
4 There are several methods that facilities can use to protect students and staff while conducting temperature and symptom screenings. The most protective methods incorporate social distancing (maintaining a distance of six feet from others) or physical barriers to eliminate or minimize exposures due to close contact. Schools should decide how to enact daily health screening, whether by active onsite screening, assessment at home by parents/guardians with daily attestation, or other method. For more information on screening, see the CDC guidance.
Every day, ask staff, parents, guardians, and students (grades 6-12) to review the following questions and stay home if the answer is yes. 1. Do you have any of the following symptoms that are not caused by another condition? [On the first day after a break or for a new student, please ask about the past 3 days 92 hours).] • Fever (100.4°F) or chills • Cough • Shortness of breath or difficulty breathing • Unusual fatigue • Muscle or body aches • Headache • Recent loss of taste or smell • Sore throat • Congestion or runny nose • Nausea or vomiting • Diarrhea 2. Have you been in close contact with anyone with confirmed COVID-19? 3. Have you had a positive COVID-19 test for active virus in the past 10 days? 4. Within the past 14 days, has a public health or medical professional told you to self-monitor, self-isolate, or self-quarantine because of concerns about COVID19 infection? For those who answer yes, refer to “Returning to school after suspected COVID-19 symptoms” below.
Reducing Transmission Grouping Students Create cohorts or groups of students with dedicated staff who remain together throughout the day, at recess and lunch time, and remain consistent from day to day. Groups should not be combined (e.g. for lunch or recess). If possible, rotate teachers rather than students to avoid mixing of students in the hallways. Consider block schedules to minimize mixing among 5 students or combining of groups.
For all students, assign seating in classrooms to be able to more quickly identify close contacts of COVID-19 cases when they occur. Multiple groups of students may use the same facility as long as they are in limited contact with other groups. Physical Distancing Practice physical distancing of six feet within each group or classroom of students as much as possible. Create space between students and reduce the amount of time they are close with each other. Your ability to do this will depend on students’ ages and developmental and physical abilities.
Select strategies to increase physical distancing that will work for your school and the space available. Maintaining six feet of distance is most important when students or staff will be engaged in something for more than a few minutes, like during class, reading or quiet time, or eating lunch. There may be brief moments, such as passing by others in the hallway or during play at recess when students are less than feet apart from each other. Not all strategies will be feasible for all schools. Think creatively about all opportunities to increase physical space between students during all scheduled activities and limit interactions in large group settings.
Schools may consider physical distancing strategies such as: • Increase the space between desks and assign seating in all grade levels and classes. Rearrange student desks or workstations to provide six feet of distance between students. Turn desks to face in the same direction (rather than facing each other) to reduce transmission caused from virus-containing droplets (e.g., from talking, coughing, sneezing). • Reduce the number of students at tables, lab benches, or other workstations to increase physical distance. • Reduce the number of students in the halls and restrooms at one time. Stagger release of classes, restroom breaks, recess, etc. Cancel activities where multiple classrooms interact. • Reduce congestion in the health office. For example, use the health office for children with flu-like symptoms and a satellite location for first aid or medication distribution. • Mark traffic flow and designate entrances and exits to minimize face to face contact. • Stagger arrival and/or dismissal times.
These approaches can limit the amount of close contact between students in high-traffic situations and times. • Place tape, spots, cones, paint or other markers to signal six feet in areas where students may be waiting in line. This could include symptom screening points, restrooms, water fountains, hand washing or sanitizing stations, the main classroom door, the cafeteria, etc. • Limit the presence of volunteers for classroom activities, mystery readers, cafeteria support, and other activities. • Cancel or modify classes where students are likely to be in very close contact. • Cancel in person activities that are considered high risk. These include choir, playing of wind instruments (band), contact sports, or other activities that require students to remove face coverings and/or be in close contact with one another as these may contribute to transmission of COVID-19.
6 • Cancel in person field trips, assemblies, and other large gatherings. Cancel in-person activities and events such as field trips, student assemblies, special performances, STEAM fairs, school-wide parent meetings, or spirit nights. • Limit cross-school transfer for special programs. For example, if students are brought from multiple schools for special programs (e.g., music, robotics, and academic clubs), consider using distance learning to deliver the instruction or temporarily offering duplicate programs in the participating schools. • Teach staff, students, and their families to maintain distance from each other in the school. Educate staff, students, and their families at the same time and explain why this is important. • Keep students outside more, as weather and space permit.
Meals Limit gatherings and potential mixing of classes or groups in the cafeteria or other communal spaces. Consider having students take their meals outside or in the classroom. You may accomplish this through meal delivery to classes, or through grab-and-go services. If using the cafeteria, have students sit with their class or group, and ensure physical distance between students in a group or cohort and between groups. Stagger meal times in lunchroom or dining hall.
Arrange and direct the flow of students to reduce crowding such as at handwashing sinks, food vending areas, etc. Space students as far apart as you can at the table. Make sure tables are at least six feet apart. Individually plate food for each student. The staff (not students) should handle utensils and serve food to reduce spread of germs. Clean and sanitize tables before and after each group eats. Use a washable plastic table cloth for wooden tables. Hygiene Practices Children and adults should clean hands when they arrive at school, before meals or snacks, after outside time, after going to the bathroom, after blowing nose or sneezing, and before leaving to go home. Help young children to make sure they are doing it right. The best option is to wash hands with soap and water for at least 20 seconds. If soap and water are not readily available, use an alcohol-based hand gel with at least 60 percent alcohol and preferably fragrance-free. Supervise use of alcohol-based hand gel by young children. Teach children and adults not to touch their eyes, nose, and mouth with unwashed hands. Cover coughs or sneezes with a tissue, throw the tissue in the trash, then clean hands with soap and water or hand gel. Cloth Face Coverings
7 Wearing cloth face coverings may help prevent the spread of COVID-19 and is required for staff and students in all public spaces, except where specific exceptions are made based on age, development, or disability. See the Washington State Department of Health Guidance on Cloth Face Coverings and CDC Recommendation Regarding the Use of Cloth Face Coverings for more information. All students, volunteers, or guests must wear cloth face coverings or acceptable alternative at school when indoors. Schools should provide face coverings for staff and students if they do not have their own. For staff, cloth facial coverings must be worn by every individual (except as described below) not working alone at the location unless their exposure dictates a higher level of protection under Department of Labor & Industries safety and health rules and guidance. Refer to Coronavirus Facial Covering and Mask Requirements for additional details.
1. Cloth face coverings should not be worn by: o Those with a disability that prevents them from comfortably wearing or removing a face covering. o Those with certain respiratory conditions or trouble breathing. o Those who are deaf or hard of hearing, and those who provide instruction to such people, and use facial and mouth movements aspart of communication. o Those advised by a medical, legal, or behavioral health professional that wearing a face covering may pose a risk to that person.
2. In rare circumstances when a cloth face covering cannot be worn, students and staff may use a clear face covering or a face shield with a drape as an alternative to a cloth face covering. If used, face shields should extend below the chin, to the ears, and have no gap at the forehead.
3. Younger students must be supervised when wearing a face covering or face shield and may need help putting them on, taking them off, and getting used to wearing them.
4. Even when cloth face coverings are worn, continue practicing physical distancing.
5. Students may remove face coverings to eat and drink and when they go outdoors for recess, physical education, or other outside activities when they can be physically distanced. If students need a “mask break” take them outside or to a large, well ventilated room where there is sufficient space to ensure more than six feet of physical distance between people.
6. As for all assistance provided by staff to students who have special needs, the school is responsible for providing appropriate PPE available. Bus Transportation Principles for COVID prevention within school transportation are: • Keep riders as far apart as possible on the bus. Consider how to reduce occupancy and increase space on the bus through scheduling (e.g., through staggered arrivals/departures, A/B scheduling) or add buses where possible • Require assigned seating • If possible, seat with household members or members of their school group/cohort
8 • Maximize outside air and keep windows open as much as possible • Encourage walking or biking where safe, or being driven by caregivers as feasible • Riders and staff members must wear a cloth face covering or acceptable alternative • Encourage students to wash or sanitize hands when they leave their home or classroom immediately before boarding the bus • Clean and disinfect frequently touched surfaces, including the tops and backs of seats, using an EPA registered product and use manufacturers’ instructions for use. Cleaning and disinfecting procedures Schools should have infection control plans, updated to reflect what is known about COVID19.
A good resource is Cleaning for Healthier Schools – Infection Control Handbook 2010 Increase how often you clean. • Cleaning removes germs, dirt, food, body fluids, and other material. Cleaning increases the benefit of sanitizing or disinfecting. • Sanitizing reduces germs on surfaces to levels that are safe. • Disinfecting kills germs on surfaces of a clean object. • The U.S. Environmental Protection Agency (EPA) regulates sanitizer and disinfectant chemicals.
If you sanitize or disinfect without cleaning first, it will reduce how well these chemicals work and may leave more germs on the surface. Current guidance for cleaning and disinfection for COVID-19 from the CDC states that disinfectants should be registered by the EPA for use against the COVID-19. See List N: Disinfectants for Use Against SARS-CoV-2 (COVID-19). Disinfectants based on hydrogen peroxide or alcohol are safer. The University of Washington has a handout with options for safer cleaning and disinfecting products that work well against COVID-19. If you use a bleach and water mixture for disinfection, mix it at a concentration of four teaspoons of 6 percent bleach per quart of cool water or five tablespoons of 6 percent bleach (one-third cup) per gallon of cool water (1,000 parts per million). Thoroughly clean surfaces with soap and water and remove the soap with water before applying the bleach solution. Keep the surface wet for at least one minute. An emergency eye wash station is required where bleach is mixed from concentrate. More information about cleaning, disinfecting, and choosing safer products is on the DOH COVID-19 website .
Clean and sanitize toys, equipment, and surfaces in the program space. Clean and disinfect high-touch surfaces like doorknobs, faucet handles, check-in counters, and restrooms. Use alcohol wipes or 70% isopropyl alcohol to clean keyboards and electronics. Outdoor areas generally require normal routine cleaning and do not require disinfection. Wash hands after you clean. If groups of students are moving from one area to another in shifts, finish cleaning and disinfecting before the new group enters the area. Clean and disinfect high-touch surfaces each night after students leave. 9 Always follow the disinfectant instructions on the label: • Use disinfectants in a ventilated space. Heavy use of disinfectant products should be done when children are not present and the facility should air out before children return. • Use the proper concentration of disinfectant. • Keep the disinfectant on the surface for the required wet contact time. • Follow the product label warnings and instructions for PPE such as gloves, eye protection, and ventilation. • Keep all chemicals out of reach of children. •
Facilities must have a Safety Data Sheet (SDS) for each chemical used in the facility. • Parents, teachers, and staff should not supply disinfectants and sanitizers. Carpets If possible, vacuum daily (when children are not present). Use a vacuum with a HEPA (high efficiency particulate air) filter – or use HEPA vacuum bags. Having both is even better. Outdoor Areas Outdoor areas, like playgrounds in schools and parks, generally require normal routine cleaning, but do not require disinfection. • Do not spray disinfectant on outdoor playgrounds—it is not an efficient use of supplies and is not proven to reduce risk of COVID-19 to the public. • High-touch surfaces made of plastic or metal, such as grab bars and railings, should be cleaned routinely. • Cleaning and disinfection of wooden surfaces (play structures, benches, tables) or groundcovers (mulch, sand) is not recommended.
Ventilation Ventilation is important to have good indoor air quality. Offer more outside time, open windows often, and adjust the HVAC system to allow the maximum amount of outside air to enter the program space. Use of fans for cooling is acceptable. They should blow away from people. There is no special cleaning or disinfection for heating, ventilation, and air conditioning (HVAC) systems. Shared Hands-On Teaching Materials Clean and disinfect hands-on materials often and after each use. Limit shared teaching materials to those you can easily clean and sanitize or disinfect.
Children’s books and other paper-based materials are not high risk for spreading the virus. 10 What to do if someone develops signs of COVID-19 To prepare for the potential of student or staff showing symptoms while at school, schools should have a response and communication plan in place that includes communication with staff, families, and their local health jurisdiction. Schools should prepare for providing instruction to students who are excluded from school due to illness, and to quarantine after exposure to COVID-19.
Every school should have an identified space for isolating ill persons until they can be sent home. This space would ideally have several rooms with doors that can close and windows that vent to the outside to improve ventilation. Alternatively, a room with several cots spaced at least six feet apart with privacy curtains between cots could be used. Ideally, the isolation unit would have a private bathroom for use only by persons being evaluated for COVID. If private bathroom for ill persons is not available, the ill person should wear a face mask when traveling to and from the communal bathroom. Clean all high touch areas between patient room and bathroom as well as in the bathroom.
Thoroughly clean and disinfect the communal bathroom immediately after use. Increase ventilation in the bathroom by keeping a window open and/or turning on a fan that vents to the outside. If a student or staff member develops signs of COVID-19 (see list under health screenings on page 3), separate the person away from others, with supervision at a distance of six feet, until the sick person can leave. Staff caring for ill persons should use appropriate medical grade PPE. While waiting to leave school, the individual with symptoms should wear a cloth face covering or mask if tolerated. Air out and then clean and disinfect the areas where the person was after they leave. Returning to school after having suspected signs of COVID-19 For ill persons without known exposure to a confirmed COVID-19 cases, follow DOH guidance for what to do if you have symptoms for COVID-19 and have not been around anyone who has been diagnosed with COVID-19. • If PCR testing for COVID-19 is not performed, stay home for at least 10 days after symptom onset, and at least 24 hours after fever has resolved and symptoms have improved. (People with severe disease or immunocompromised may need to be isolated at home for longer.) •
If PCR testing for COVID-19 is negative, stay home until 72 hours after fever resolves and symptoms are improving. People who are ill and had known exposure to a person with confirmed COVID-19 should be encouraged to be tested for COVID-19 and should stay out of school until at least 10 days after symptom onset, and at least 24 hours after fever has resolved and symptoms have improved. (People with severe disease or immunocompromised may need to be isolated at home for longer.)
Ask staff and students’ parents or caregivers to inform the school right away if the ill person 11 is diagnosed with COVID-19. If a student or staff member tests positive for COVID-19, the local health jurisdiction will provide advice, but it is possible that many of the student’s classmates and teachers will be considered close contacts and need to be quarantined for 14 days. Refer them to What to do if you were potentially exposed to someone with confirmed coronavirus disease (COVID- 19)? Returning to school after testing positive for COVID-19 A staff member or student who had confirmed COVID-19 can return to the program when: • At least 24 hours have passed since recovery – defined as no fever without the use of medications and improvement in respiratory signs like cough and shortness of breath; AND • At least 10 days have passed since signs first showed up. Returning to school after being in close contact to someone with COVID-19
If a person believes they have had close contact to someone with COVID-19, but they are not sick, they should watch their health for signs of fever, cough, shortness of breath, and other COVID-19 symptoms during the 14 days after the last day they were in close contact with the person sick with COVID-19. They should not go to work, child care, school, or public places for 14 days. If a person develops symptoms of COVID-19 during their quarantine, they should seek testing for COVID-19, and follow guidance above for confirmed COVID-19 cases. Consider testing at day 10 even if no symptoms are present. However, a negative test after exposure does not shorten the 14 day quarantine period. Environmental cleaning after a suspected or confirmed case is identified
When a school sends a person with COVID-19 symptoms home, or learns a confirmed case of COVID-19 has been on the premises, clean and disinfect the areas where the ill person spent time. • Close off areas visited by the ill persons. Open outside doors and windows and use ventilating fans to increase air circulation in the area. Wait 24 hours, or as long as practical, before beginning cleaning and disinfection. • Cleaning staff should clean and disinfect all areas such as offices, bathrooms, common areas, shared electronic equipment (like tablets, touch screens, keyboards, remote controls) used by the ill persons, focusing especially on frequently touched surfaces. • If it has been more than 7 days since the person with suspected/confirmed COVID-19 visited or used the facility, additional cleaning and disinfection is not necessary. 12 Contact investigation, contact tracing, and quarantine of close contacts of confirmed COVID-19 cases Schools can play an important role to quickly identify close contacts and communicate with parents and guardians.
When a school learns of a confirmed case of COVID-19 who was on the school premises, • Immediately notify the local health jurisdiction of the case. • Identify and provide to local public health all likely school-based close contacts of the COVID-19 case from 2 days before symptoms started (or date of positive test if asymptomatic) until the time the case was no longer in school.
Close contacts are defined as persons who were within six feet of the confirmed cases for approximately 15 minutes and would include o Siblings who attend the same school o Some or all of the students and teachers in the infected person’s group (classroom, cohort) o Others sitting close to the student on the school bus • Public health will advise close contacts, but the school may help quickly communicate important information to exposed students and staff who should be advised to selfmonitor and quarantine for 14 days from the last exposure.
Schools may use DOH guidance: What to do if you were potentially exposed to someone with confirmed coronavirus disease (COVID- 19)? COVID-19 outbreaks in school Definition: Two or more* laboratory-confirmed† COVID-19 cases among students or staff with onsets‡ within a 14-day period, who are epidemiologically linked§, do not share a household**, and were not identified as close contacts†† of each other in another setting during standard case investigation or contact tracing. If the school is grouping or cohorting students Dismiss the entire classroom for home quarantine for 14 days if two or more confirmed cases of COVID-19 occur within the group or cohort within a 14 day period.
Close a school and switch to remote learning for 14 days when • 2 or more classrooms are dismissed due to outbreaks (in schools with 10 or fewer classrooms) • >=10% of classrooms are dismissed due to outbreaks (in schools with > 10 classrooms) • School cannot function due to insufficient teaching or support staff. If the school is not grouping or cohorting students Quarantine close contacts and notify families if two or more confirmed cases are reported in a 14 day period. Evaluate to determine if transmission is occurring in the school. 13 Consider the following to determine the need to close a school and switch to remote learning for 14 days when: • Rapid increase in cases • Prolonged chain of transmission (2 or more generations) believed to occur in the school. • School cannot function due to insufficient teaching or support staff.
More COVID-19 Information and Resources Stay up-to-date on the current COVID-19 situation in Washington, Governor Inslee’s proclamations, symptoms, how it spreads, and how and when people should get tested. See our Frequently Asked Questions for more information. A person’s race/ethnicity or nationality does not, itself, put them at greater risk of COVID-19. However, data are revealing that communities of color are being disproportionately impacted by COVID-19- this is due to the effects of racism, and in particular, structural racism, that leaves some groups with fewer opportunities to protect themselves and their communities. Stigma will not help to fight the illness. Share accurate information with others to keep rumors and misinformation from spreading. (bold lettering added for emphasis.
• WA State Department of Health 2019 Novel Coronavirus Outbreak (COVID-19) • WA State Coronavirus Response (COVID-19) • Find Your Local Health Department or District • CDC Coronavirus (COVID-19) • Stigma Reduction Resources Have more questions about COVID-19? Call our hotline: 1-800-525-0127, Monday – Friday, 6 a.m. to 10 p.m., Weekends: 8 a.m. to 6 p.m. For interpretative services, press # when they answer and say your language. For questions about your own health, COVID-19 testing, or testing results, please contact a health care provider. To request this document in another format, call 1-800-525-0127. Deaf or hard of hearing
More From 870 AM KFLD